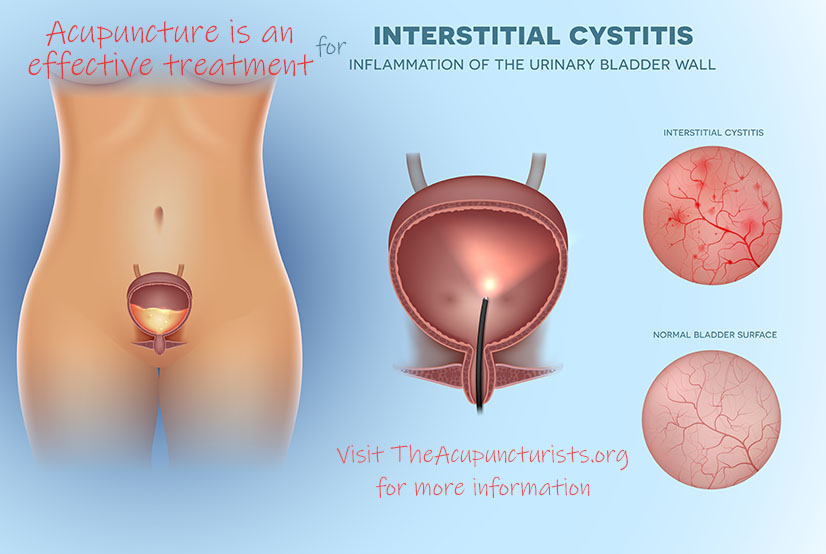
Interstitial Cystitis (IC) is an autoimmune related condition that causes discomfort or pain in the bladder and a need to urinate frequently and urgently. It is also referred to as bladder pain syndrome, (BPS) is a chronic bladder health problem affecting more than 12 million people in the United States today. Twice as many women than men are affected and it is more common in adults than in children – though anyone can get the condition (Interstitial Cystitis Association, 2016).
What is Interstitial Cystitis?
The Urology Care Foundation, which is an official chapter of the American Urological Foundation, defines Interstitial Cystitis (IC) as a chronic bladder health issue which entails pain, discomfort and pressure in the bladder area. The condition is commonly associated with urinary frequency and urgency.
The bladder is responsible for holding urine before urination once the kidneys have filtered it out; IC is a condition that makes a patient feel pain and pressure in the bladder area when the urine is being held. It causes painful and very urgent bathroom trips. In severe cases, one can pass urine 40-60 times in a day.
This condition has indicators that can be described as urinary tract symptoms which have been recurrent for more than six weeks without any positive infection traces or any other clear causes.
Symptoms of Interstitial Cystitis
The symptoms of IC can be mild or severe; they can also be constant and go away for some. Below are some of the major symptoms that need immediate attention.
- Pain – This is the major and most common symptom of IC. The pain is normally accompanied by a feeling of pressure in the lower abdomen, or the lower back, or the pelvic and perineal area and sometimes, all the areas at once. One experiences pain once their bladder fills and it could be constant or could come and go.
- Urgency – This is the urgent need to go. A feeling of being pressed all the time. For some, the urge never goes away even after passing urine. In some cases, the urgent feeling comes all at once and can worsen with time.
- Frequency – With IC, one feels the need to go to the bathroom more often than normal. As the frequency increases, so does the urgency.
People who suffer from IC point out that the severity of symptoms vary based on things like the foods and drinks they take, physical and mental stress, menstrual cycles for the women and sexual activities for both men and women.
Causes of Interstitial Cystitis
Scientists and experts have not yet unearthed the definite cause of IC but unproven theories that have been floated include:
- An element in the urine that damages the bladder.
- Defects in the bladder tissue that could allow harmful material in the urine to get to the bladder.
- An attack on the bladder from the body’s immune system.
- Presence of a mast cell, an inflammatory cell that releases chemicals that lead to IC symptoms.
Western medical approaches to Interstitial Cystitis
Medical experts approach Interstitial Cystitis treatment through symptom control. Medical practitioners often administer treatment in phases and take the approach that no one treatment option works for all. Discussed below are the treatment options offered;
Oral Medications – Oral medications that are used for treatment include:
- Non-steroidal anti-inflammatory drugs, such as ibuprofen, to relieve pain.
- Antihistamines to reduce urinary urgency and frequency and relieve other symptoms.
- Tricyclic antidepressants to relax the bladder and block pain
Bladder Instillation – This involves instilling medicine into the bladder. For this process, the doctor places medication into the bladder through a thin and flexible tube inserted through the urethra.
Physical Therapy – Physical therapy helps in relieving pain that is associated with restrictive connective tissues, muscle tenderness and any abnormalities in the pelvic floor.
Bladder Distention – Bladder distention is the process of stretching the bladder using water. Some patients will notice improvement and if it works for them in the long-term, the procedure is repeated.
Nerve stimulation – In this case, specific nerves are stimulated using various techniques to improve flow of blood to the bladder, reduce frequency and urgency to urinate. If symptoms are reduced by this procedure, the practitioner will explore the option of implanting a permanent device that will stimulate the respective nerves.
Surgery – This is a treatment method that doctors rarely opt for because of the complications that can arise after surgical procedures. Surgery is considered for patients with severe pain, patients whose quality of life has been affected and all the other treatment options have failed. Surgery is done to get rid of any ulcers that may be present with the interstitial cystitis and increase the bladder capacity. In such cases, the patients empty their bladder by means of a catheter.
Acupuncture as treatment for Interstitial Cystitis
Acupuncture is an alternative treatment that can applied to remedy interstitial cystitis. There is ample evidence that points to acupuncture being a successful treatment regimen; especially when it comes to the control of inflammation and pain encountered by IC patients. Studies have shown a great degree of success for those taking up this mode of treatment (Whitmore, 2002).
During treatment, the acupuncture practitioner identifies the imbalances in the body and an acupuncture prescription is tailored to correct the imbalance. Once this is done, acupuncture needles are placed along the identified channels so as to regulate the flow of energy. This procedure works with the theory that the needles relieve pain and other symptoms by boosting the body’s natural painkillers and correcting any other internal imbalances. This procedure corrects the root problem by encouraging the body to heal itself.
When it comes to the treatment of IC, apart from the pain relief, acupuncture is used to deal with the urgency, discomfort and any stress that comes with the condition.
Studies that Support Acupuncture as an effective treatment method for Interstitial Cystitis
A Norwegian study broke down a sample into three groups of patients. One group received acupuncture treatment, the second received sham acupuncture and the third did not receive any treatment. It was found that 85% of the participants in the group that received acupuncture were free of IC during a 6-month observational period (Aune et al.1998).
In another study of a smaller sample size, Rapkin and Kames found that 6 to 8 weeks of acupuncture reduced the pain brought about by IC (Rapkin and Kames, 1987).
Yet another study concluded that acupuncture needling combined with moxibustion improves the condition of patients with IC. During the sessions, Moxa needles were applied to acupuncture points and the patients experienced significant improvement in their condition. The patients had already been treated via conventional treatments such as pharmaceutical medications and instillations but had not responded positively. The researchers concluded that acupuncture treatment is an effective complementary and alternative therapeutic option for interstitial cystitis. (Katayama et al. 2013)
Interstitial Cystitis is a difficult and stressful condition to live with. Its symptoms can lower one’s quality of life. Western medicine has its own way of dealing with the symptoms. On its part, acupuncture works with the body’s natural energies. With successful studies and cases of this alternative regimen documented, acupuncture remains a non-invasive, effective and natural way to handle interstitial cystitis. With proper consultation, it can be used as a complementary method or an outright effective alternative all together.
The Acupuncturists, Dr. Robert Herbst and Dr. Landon Agoado, are licensed and skilled, offer free consultations and serve Margate, Coconut Creek, Coral Springs, Tamarac, Parkland, Deerfield Beach, Ft. Lauderdale and West Boca.
[DISPLAY_ULTIMATE_SOCIAL_ICONS]
References
- https://www.urologyhealth.org/urologic-conditions/interstitial-cystitis
- https://www.niddk.nih.gov/health-information/urologic-diseases/interstitial-cystitis-painful-bladder-syndrome/definition-facts
- http://www.healthcmi.com/Acupuncture-Continuing-Education-News/772-bladderub32
- Katayama, Y., K. Nakahara, T. Shitamura, S. Mukai, H. Wakeda, Y. Yamashita, K. Inoue, K. Nose, and T. Kamoto. “[Effectiveness of Acupuncture and Moxibustion Therapy for the Treatment of Refractory Interstitial Cystitis.].” Hinyokika kiyo. Acta urologica Japonica 59, no. 5 (2013): 265-269.
- Pang R, et al. The Chinese approach to complementary and alternative medicine for interstitial cystitis/bladder pain syndrome. Translational Andrology and Urology. 2015;4:653.
- Verghese, Tina S.; Riordain, Richael Ni; Champaneria, Rita; Latthe, Pallavi M. (7 December 2015). “Complementary therapies for bladder pain syndrome: a systematic review”. International Urogynecology Journal. 27 (8): 1127–1136. doi:10.1007/s00192-015-2886-3.
- Whitmore, KE (2002). “Complementary and Alternative Therapies as Treatment Approaches for Interstitial Cystitis”. Reviews in urology. 4 Suppl 1 (Suppl 1): S28–35. PMC 1476005 Freely accessible. PMID 16986031.